Exit the Swim Alive
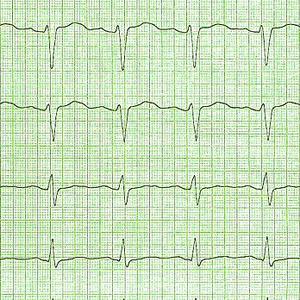
The saddest thing I experience in our great sport of triathlon is when one of our fellows commences his effort one morning eager with hope, and does not come home, safe, to his family that night. This is the one mean, hard tragedy in a sport that delivers almost unqualified benefits and blessings.
We cannot stop people from dying in triathlons, and they die both in racing and training. What we can do, I think – what we must do – is draw these deaths down to a bare minimum.
Triathlon’s national governing body in the United States, USA Triathlon, commissioned a study on this, and we summarized and commented on that study.
Our intention is to get as granular as we can about heart health and how you can avoid the sort of trouble we all know could arrive at each of our doors. To that end, what you'll read over the next week is a series written in 4 parts. Today I'll talk about basic heart health, and what I — with a big assist from the medical community that has specifically studied deaths in triathlon — think causes people to die in triathlon.
In Part 2 I'll stipulate that if I suffer cardiac arrest during the swim I may well have an underlying heart ailment. However, if I die in the swim, why did I die, on that day, in the swim? Why not the night before? The night after? Or during the run? Something clearly happens in the swim. I'll write about habits and behaviors that I believe will help reduce the triggers of cardiac arrest while swimming.
In Part-3 I won't really be writing to you, reader, I'll be writing to those who put on the races you enter. But you're welcome to eavesdrop.
And in Part 4 I'll circle back to what we're writing about today. I'll announce a pilot program, in one metro area, for triathletes, in conjunction with a cardiac practice, whereby you can very inexpensively do everything you can to make as certain as you can that your heart is ready for the training and racing we all contemplate.
ETIOLOGIES
Please pardon my bluntness here; I just want to be very clear what's going on. If you have a heart attack or cardiac arrest while driving, and this causes you to run into a fixed pole at 70mph, and you die on impact, the cause of death may be the blunt force trauma. But the proximate cause of that death is the heart problem. If you die in the swim leg of a triathlon, unless it's as you're exiting the water (which happens) you will technically drown. However the proximate cause will be the heart condition, and this is almost always what kills triathletes during the swim leg (one can then ask, well, what was the proximate cause of the heart attack? We'll get to that in Part 2).
One hypothesis is that…
There was an imbalance (at some point during the race) between the supply and demand of coronary blood flow, in the presence of a fixed obstruction, that resulted in an oxygen-deprived region of the heart that precipitated an arrhythmia.
I borrowed this elegant description of a heart attack from Dr. Lawrence Creswell, who I'll reference below.
In other words, in plumbing terms, either there was a blockage in the pipe, or the pipe was too small. Let's just say, for the purpose of discussion, that the pipe was too small for the requisite work. If I just keep adding sprinklers to the irrigation line without supplying more water through a larger pipe, each sprinkler head will simply deliver an anemic spray. Why doesn't the heart just do that? Why does it throw a tantrum, in the form of a heart attack?
Usually, the small anemic sprinkler head spray is what happens in our bodies. I slow down. I slow down more. I stagger. Maybe I faint. Hopefully I stop well before then. But I don't have a heart attack. Unfortunately, the cascading effect of too little oxygen for the required work sometimes does cause the heart to throw a catastrophic tantrum, and that's usually because there's something about that specific heart that is anomalous, and this anomaly interferes with the electrical impulses that cause the heart to beat.
If cardiac arrest is the proximate cause of drowning in most of these triathlon swim deaths, what is the proximate cause of the fatal arrhythmia? We'll get to that.
YOUR VERY FIRST STEP
What you want is a how-to. “Just tell me what to do, so that I have my best chance of staying alive.” I know this is what you’re asking, because a lot of you have voiced this imperative in one way or another. So, here you go:
What you need is a resting EKG, along with a short analysis of your symptoms and history by a doctor. You don’t necessarily need to do this annually, although annually is very good. But you absolutely do need to do this once.
First, what are these tests? An EKG is the same thing as an ECG. It measures the electrical activity of your heart. These acronyms are short for electrocardiogram.
This is distinct from an echocardiogram. While the former measures the electrical behavior of your heart, the latter is an ultrasound of your heart. It’s just like when you fathers look at your babies in your wives’ tummies, just, move a little higher — over your heart — and that’s what I’m talking about. During an echocardiogram your doctor is bouncing sound waves off your heart, just like a submarine’s sonar, just like the echolocation of a bat or a whale. You can’t hear these sound waves because they are sent out at a frequency too high for your ears to detect.
An echocardiogram is not the first line test. But an echo can discover holes in your heart, or heart valve problems, aortic aneurisms, enlargement of the heart or thickening of the ventricular walls. An echo is handy, but it’s probably twice as expensive as an EKG, and sits behind the EKG in its value as a cost-effective first line of clinical defense.
These are two very non-invasive and (in the grand scheme of things) not very expensive procedures. If you have not had an EKG during your adult life, the first EKG you get is an order of magnitude more important than any subsequent ones, because the first may well uncover congenital problems, or be sufficiently questionable to cause you to move toward an echocardiogram that might shed further light on your heart health.
CONGENITAL HEART DEFECTS
If you are in your 20s or 30s and you're still alive — which is a pretty sound bet if you're reading this — you may have a congenital heart defect that has not manifested itself yet. If it does manifest itself, you and I probably won't be discussing this. The evidence so far suggests that those who have died of cardiac arrest during an endurance event in your age range tend more likely to die from congenital heart problems, rather than from heart disease acquired or accumulated since then. The idea is for you to identify this prior to doing something that would trigger a fatal occurrence.
What are these congenital defects? Two in particular are hypertrophic cardiomyopathy (HCM), and prolonged or long QT syndrome. Your garden variety EKG is a pretty good front line test to ferret these out. As noted, just an EKG one time will solve the mystery of whether you have these inherited problems.
But those aren’t the only possibilities. Your coronary arteries might have an abnormal anatomy from birth. Or you might have a bicuspid aortic valve or an aortic aneurism, and these sorts of things have stopped athletes short of a fatal cardiac event: Normann Stadler and Torbjorn Sindballe come to mind. These sorts of structural problems can be identified with an echocardiogram.
CORONARY ARTERY DISEASE (CAD)
This is another animal altogether. Unfortunately, problems like coronary artery blockages are not as easily identified through these easy tests. They require more extensive testing.
I had a bout with atrial fibrillation several years back, and as a result of this I underwent a nuclear stress test. A radioactive isotope was injected into an artery, and then I ran on a treadmill. A special (gamma) camera photographed my chest, and if a part of my heart did not show up on film that meant that my arteries did not supply any or enough blood to that part of my heart. Because my entire heart “glowed” that meant my nuclear blood made it to all its chambers. There are several ways to “image” the heart during exercise: the way mine was done, via sound waves (stress echo) or via electrical impulses (stress EKG).
These are the sorts of tests you’d get if you exhibit symptoms of CAD, and those symptoms might be shortness of breath, fainting, or chest pain. If you feel this during workouts, and your standard EKG came back clean, you should consider testing that would identify CAD. I’ve had some very good friends — very good, very fit athletes — who notwithstanding their fitness suffered from significant coronary blockages that would very likely have led to a heart attack if left undiagnosed. Keep in mind, this is not rare; CAD is in fact is the leading cause of death worldwide. Two dear friends each experienced symptoms during workouts (one while riding, one during his swim workout). They each immediately went to the emergency room, each received requisite testing, and after only moderately invasive “plumbing” procedures each is back working out full steam today.
CONTROVERSY
If you look at the recommendations of the American Heart Association, and you look at what is considered the state of the art in smart, effective heart health screening in Europe — in Italy in particular — you'd conclude that each continent is looking at different sets of data. The AHA does not believe that an EKG (ECG) is a very reliable predictor of sudden cardiac arrest. "Current U.S. recommendations don’t include ECGs," it says, "most notably due to a lack of policy mandate and infrastructure to support this."
I find that last phrase illustrative. I conclude — based just on what I've read from the AHA — that it is writing this in the context of the sort of mass screening that would be needed for all sports, including high school sports. My sense, while trying to divine the AHA's meaning, is that there is not the political will to fund a program to expertly administer and analyze 5 million EKGs a year to everyone, high school and up, who wants to participate in an athletic event.
Conversely, the experience in Italy is that sudden cardiac death during athletic events has decreased 89 percent since the required administration of EKGs as a prerequisite to athletic activity.
That said, even those cardiologists to whom I've spoken who err on the side of EKGs and associated clinical tests tell me that there are false positives, as well as "false negatives," that is, these EKGs, echoes, stress EKGs and echoes, may in the end be only 50 or 70 percent predictive of a heart anomaly.
I can't square this circle.
I choose to look at it this way: When I leave the house, I put on a helmet, I turn on the bike light, I check my bike for problems, I choose a safe route, I hike my leg over my bike, and I commence riding knowing that I've done all I can, but there is no certain armor shielding me from bad things happening.
Leveraging that premise — doing all I reasonably can, knowing that there is no inoculant protecting me from sudden cardiac death — what you'll read in Part 4 of this series is the announcement and description of a program that will not save every life, but might save some. It's a low-cost, nuts-and-bolts, program of examination and testing that incorporates clinical testing, and questions and protocols from the American Heart Association's 12-point protocol and the Framingham Heart Study.





